

Stroke and Neuroplasticity


Stroke and Neuroplasticity
Stroke
is the most common neurological disease that affects the nervous system
and it is also the principal cause of mental and physical disabilities.
It happens due to an interruption in the blood stream to the brain, this
interruption can happen like an obstruction of the artery that supplies
the brain - the so-called ischemic stroke,
or by the rupture of a vessel - the hemorrhagic
stroke.
The most important cause related to stroke are: high blood pressure, diabetes mellitus, heart diseases, fat, sedentariness and smoking.
The consequences depend on: the location,
the affected brain areas size, and the time passed from its occurrence
until the patient assistance (the quicker the recovery starts, the better
is the prognosis). The most common sequel are hemiplegia and visual, speaking
and memory alterations.
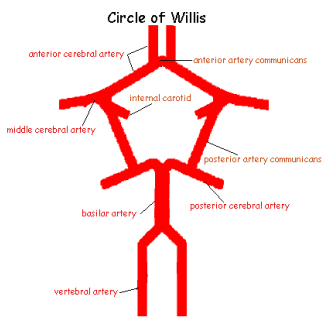
The blood reaches the brain through
the vertebral artery and the internal carotid artery. Both arteries communicate
each other through the Circle of Willis.
This is an arterial anastomosis that provides blood supply to the brains
hemispheres, and it is formed by the anterior cerebral arteries, the posterior
cerebral arteries, the anterior artery communicans, the posterior arteries
communicans and the internal carotid. These arteries have very thin walls,
that makes them more vulnerable to hemorrhages. The cerebral artery most
affected by a stroke is the middle cerebral artery.
The recovery of functions of the limbs
which is promoted by plasticity is more difficult to occur, due to a phenomenon
known as learned non use. With the loss of a brain areas function, the
body part that was linked to this area is also affected and its mobility
power is lost too. As the patient cannot move his most affected limb, he
compensate this using the other limb. Thus, after a certain period, when
the damage effects arent present anymore and brain readaptations happen,
the movements could be recovered, but the patient has already learned
that the limb is no longer functional.
This technique consists in the forced use of the affected arm by the limited use of the non-affected arm. During a 10 to 15 days period, the patients non-affected arm is immobilized. Consequently, many activities like dressing, eating, writing, cooking, etc. can only be done by the affected arm, stimulating the damaged cortex. In this period, the patient has a six daily hours of physiotherapy training, doing repetitive tasks with the affected arm. Due to this increased use of the affected arm, the brain area connected to it is stimulated once again and occurs an intense cortical reorganization. This reorganization increases the representation area of this limb in the cortex and the motor function ability is improved. So the CI-therapy can be considered remarkably effective against the learned nonuse .

Liepert, J., Bauder, H., Miltner, W. H. R., Taub, E., Weiller, C. (2000). Treatment-Induced Cortical Reorganization After Stroke in Humans. Stroke 31: 1210-1216
Liepert, J., Miltner, W.H.R., Bauder, H., Sommer, M., Dettmers, C., Taub, E., Weiller, C. (1998). Motor cortex plasticity during constraint-induced movement therapy in stroke patients. Neurosci Lett. 250:58.
Taub ,E., Uswatte, G., Pidikiti,
R.D. (1999). Constraint-induced movement therapy. a new family of techniques
with broad application to physical rehabilitation-a clinical review. J
Rehab Res Dev. 36: 237251.
 Mirella
Magalhães Tenório Brito, undergraduate in Physiotherapy at
UFPE, monitor at Anatomy 1, apprentice at Hospital das Clínicas
de Pernambuco in Orthopaedic Trauma, and scientific research beginner in
Neurophysiology and Pathology. E-mail: mirellabritto@hotmail.com
Mirella
Magalhães Tenório Brito, undergraduate in Physiotherapy at
UFPE, monitor at Anatomy 1, apprentice at Hospital das Clínicas
de Pernambuco in Orthopaedic Trauma, and scientific research beginner in
Neurophysiology and Pathology. E-mail: mirellabritto@hotmail.com
 Nicodemos
Teles de Pontes Filho, MD in Imunopathology at UFPE, PhD student in Nutrition.
Professor of Pathology Department, special researcher of LIKA ( Keizo Azami´s
Imunopathology Laboratory-UFPE), with specialization in Eletronic Microscopy
at Keio University, Japan.
Nicodemos
Teles de Pontes Filho, MD in Imunopathology at UFPE, PhD student in Nutrition.
Professor of Pathology Department, special researcher of LIKA ( Keizo Azami´s
Imunopathology Laboratory-UFPE), with specialization in Eletronic Microscopy
at Keio University, Japan.